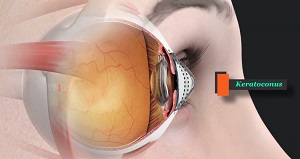
What is Keratoconus?
Keratoconus is an eye condition in which the shape of your cornea, the clear, dome-shaped structure present in front of your eye, is changed. The condition causes the cornea to become thinner and gradually bulge outward in the shape of a cone. Keratoconus is usually a progressive condition that can affect one eye or both eyes at the same time.
Causes of Keratoconus
These factors can increase your chances of developing keratoconus:
- Family history
- People aged between their late teens and 30 years of age
- Rubbing your eyes vigorously
- Certain conditions, such as retinitis pigmentosa, Down syndrome, Ehlers-Danlos syndrome, Marfan syndrome, hay fever and asthma
- Eye infections
- Allergic reactions
- Persistent use of chemical eye irritants or any aesthetic applicants
Symptoms of Keratoconus
Symptoms of keratoconus may change as the disease progresses. They include:
- Blurred or distorted vision
- Hypersensitivity to bright light and glare, causing problems with night driving
- Vision impairment
- Frequent vision changes requiring you to change your eyeglass or lens
- Sudden worsening or cloudy vision
- Redness of the eye
- Swelling in the eye
- Double vision
Diagnosis of Keratoconus
Your ophthalmologist will review your medical or family history and conduct a thorough eye examination. Further specialized eye tests may be done to find out more about the shape of your cornea and confirm a diagnosis of keratoconus such as:
- Eye Refraction Test- During this test, you may be asked to look through a device called a phoropter which contains different lens. This device helps to judge which combination of lenses can give you the sharpest vision. You doctor may also use a hand-held instrument called a retinoscope to evaluate your eyes.
- Slit-lamp examination- During this test a vertical beam of light is directed on the surface of the eye by using a low-powered microscope to view the eye. This helps your doctor evaluate the shape of your cornea and look for other potential problems in the eye.
- Keratometry- During this test, a circle of light is focused on the cornea to measure the reflection that helps to identify irregularity in the shape of the cornea.
- Computerized corneal mapping- Advanced photographic tests, such as corneal tomography and corneal topography are used to create detailed images of the shape, size, and thickness of the cornea.
Treatment of Keratoconus
Treatment for keratoconus depends on the severity of your condition and progression of the disease. The following are some of the treatment options:
Nonsurgical Options
The various nonsurgical options include:
- Eyeglasses or soft contact lenses- In the early stages of the disease when your symptoms are mild, your vision can be corrected with eyeglasses or soft contact lenses which can correct blurry or distorted vision.
- Hard contact lenses- Hard contact lenses include rigid and gas permeable options that are used in treating more-advanced keratoconus. They may feel uncomfortable at first but they provide excellent vision and you will get used to wearing them gradually.
- Corneal cross-linking- During this procedure, the cornea is saturated with eye drops and treated with ultraviolet light. This causes cross-linking of the cornea, which will stiffen preventing further shape changes. Corneal cross-linking may help to reduce the risk of progressive vision loss by stabilizing the corneal shape in the early phase of the disease.
Surgical Options
The various surgical options include:
- Intacs- This is a small curved device that is placed in your cornea by your ophthalmologist surgically. Intacs help flatten the curvature of your cornea to improve vision.
- Intrastromal corneal ring segments (ICRS)- To treat mild-to-moderate keratoconus, your ophthalmologist may surgically insert small synthetic rings in your cornea. This treatment can help flatten the cornea, which may help improve vision and make contact lenses fit better.
- Corneal transplant- When symptoms are severe and there is cornea scarring observed, your ophthalmologist may suggest a corneal transplant. During this procedure, your ophthalmologist replaces all or part of your affected cornea with healthy donor cornea tissue. The procedure is also known as keratoplasty.
Prevention of Keratoconus
Some of the common preventive measures to avoid keratoconus includes:
- Avoiding frequent rubbing of your eyes
- Careful use of contact lenses to avoid scarring of the cornea
- Eye exercises
- Healthy diet
- Adequate sleep
- Washing your eyes everyday with clear water
- Regular checkups with your ophthalmologist if you have symptoms or a family history of the condition
For more information about our services or to schedule an appointment, call us at or request an appointment online. We’ll respond to you as soon as possible.







